News
News
A PEEK INTO OUR PROCESS
On The Boards
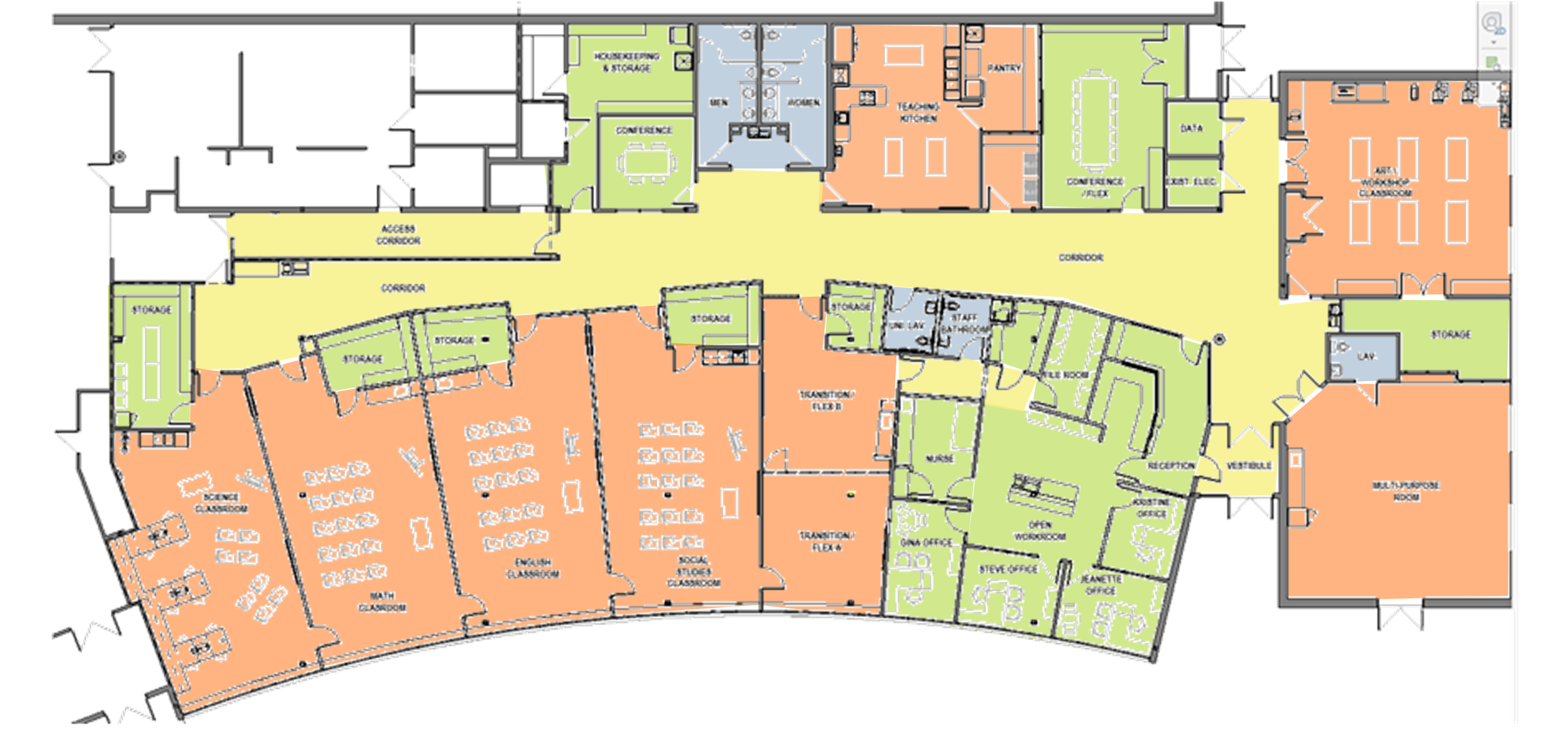
The JSA team shadowed the students and staff of Gammon Academy, gaining a deep understanding of the requirements for educating and nurturing the students with neurobehavioral, developmental, and/or intellectual challenges.
We are revitalizing the building originally owned and occupied by the Margeson Bros Furniture Co., bringing a new level of sophistication as it becomes the Novocure corporate headquarters.
The acquisition of Community Campus by the City of Portsmouth offers Robert J Lister Academy the chance to transition from its outdated building into purposefully renovated and updated spaces.
ALL THINGS ARCHITECTURE & DESIGN
Insights
Renovating an architecturally-significant skilled nursing and rehab facility requires careful planning and creativity.
In a new white paper, Sandra Hodge, IIDA and Robin Tufts, AIA describe JSA's research into designing healthy environments for vulnerable populations.
We feel trapped in our homes, unable to go out to connect with friends or grab a bite to eat at any number of restaurants. We’re secluded, shut off from our communities, fearful this won’t end.
STAY IN THE KNOW
Company Updates
We're working with longtime client Portsmouth Regional Hospital to add a new cesarean section operating suite to its labor and delivery unit. The $1.3 million renovation is expected to be completed in spring 2023. Read more about the project
We received the 2022 Rick and Duffy Monahon Award for Design Excellence in Architectural Restoration and Preservation from AIANH for our work on 3 Pleasant Street, a historic mixed-use property in downtown Portsmouth, NH.
Anne Weidman, director of community engagement and business development, was honored as a "life changer" by HAVEN, New Hampshire's largest violence prevention and support services agency, at their annual Changing Lives event on October 13.